Member-only story
The Impact of Police Brutality on Covid-19 and Medical Mistrust
Violence in law enforcement is affecting trust in medicine when it’s needed the most
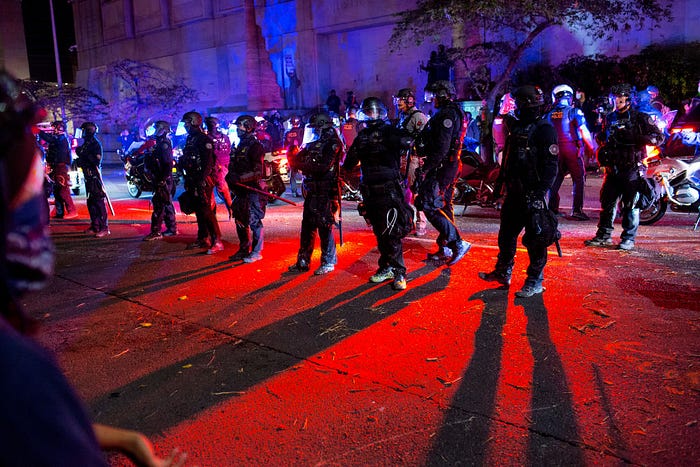
Last week, a grand jury’s decision not to charge any of the police officers who killed Breonna Taylor set off a new wave of protests against racist police brutality across the United States. The protests have been ongoing since May, when a Black man named George Floyd was murdered by a police officer in Minneapolis.
Meanwhile, the Covid-19 pandemic has raged on, and people of color, especially Black people, have disproportionately felt its effects. Across the United States, Black people are dying at 2.3 times the rate of white people, according to the Covid-19 Racial Data Tracker. As the Coronavirus Blog previously reported, this gross disparity is due to a number of factors affecting Black people, including economic inequality, health care disparities, and redlining, a racist U.S. housing policy that pushed people of color into less desirable neighborhoods.
Another reason for the disproportionate impact of Covid-19 on Black people and people of color may be police brutality itself. In January of this year, a team of researchers led by Lehigh University’s Sirry Alang, PhD, an associate professor of sociology and health, medicine, and society, published a study revealing the links between police brutality and mistrust in medical institutions in the Journal of Racial and Ethnic Health Disparities. This study showed that people of all racial groups who had negative encounters with the police had higher levels of medical mistrust than people who didn’t have negative encounters. And this held true even if people thought the negative encounters were necessary.
Public awareness of police brutality has increased since the start of the Black Lives Matter protests in May. And this, Alang tells the Coronavirus Blog, can have an impact on the way Black people are handling the pandemic.

